One of the most common questions I hear from parents during consultations is whether their child can continue playing sports during orthodontic treatment. The short answer is absolutely yes. I have treated soccer players, basketball stars, wrestlers, swimmers, gymnasts, and every other type of athlete you can imagine. Being active and playing the sports you love should not stop because you have braces. But it does require some smart precautions, and that is what I want to talk about today.
Playing Sports with Braces
Can you play sports with braces? Yes, without question. Millions of athletes around the world compete at every level, from youth recreational leagues to professional sports, while wearing braces or aligners. The presence of orthodontic hardware does not disqualify you from any sport, nor does it need to limit your performance in any meaningful way.
That said, orthodontic appliances do change the equation when it comes to facial injuries. Braces have brackets and wires that sit against the inner surface of your lips and cheeks. If you take a hit to the face, whether from a ball, an elbow, or a fall, those brackets can cut into soft tissue. The teeth themselves may also be slightly more vulnerable during active treatment because they are being intentionally loosened as part of the movement process. This does not mean your teeth are going to fall out if you get bumped, but it does mean that protecting your mouth becomes more important.
The Mouthguard Question
Do you need a mouthguard with braces? I tell every single one of my patients who plays any contact or collision sport that a mouthguard is essential. In my view, it is not optional. A mouthguard protects the soft tissues of your mouth from being lacerated by brackets and wires during impact. It also absorbs and distributes force, reducing the risk of broken teeth or damage to the orthodontic appliances themselves.
Even for non-contact sports, I recommend a mouthguard if there is any chance of a fall or a collision. Basketball is technically non-contact, but anyone who has played knows that elbows fly regularly. Soccer involves heading the ball, and accidental head-to-head contact is common. Skateboarding, mountain biking, volleyball: all of these carry risks that a mouthguard can mitigate.
Choosing the Right Mouthguard
Not all mouthguards are created equal, and this is especially true for orthodontic patients. The standard boil-and-bite mouthguards you find at sporting goods stores are designed to mold tightly around the teeth. For someone in braces, this creates a problem. A tight-fitting mouthguard made at the start of treatment will not fit properly as teeth move. Worse, it could actually interfere with tooth movement or damage brackets.
The best option for orthodontic patients is an orthodontic-specific mouthguard. These are designed with extra room in the front to accommodate brackets and wires. They fit more loosely around the teeth because they need to allow for ongoing movement. Some are available over the counter in an orthodontic design, and others can be custom-fabricated by your local orthodontist for a better fit.
I typically recommend a thicker, orthodontic-style mouthguard for my patients in full contact sports like football, hockey, and lacrosse. For sports with moderate risk, a standard orthodontic over-the-counter guard works well. The key is that it should cover all the brackets, sit comfortably, and allow the patient to breathe and speak without too much difficulty.
What to Do If You Take a Hit
Despite our best efforts at prevention, injuries happen. If you or your child takes a hit to the mouth during sports while wearing braces, here is what I recommend. First, assess the situation calmly. Check for any loose teeth by gently pressing on them with a finger. Look for broken brackets or poking wires. Examine the lips, cheeks, and gums for cuts.
If a bracket has come loose but is still attached to the wire, it is not an emergency. Call your orthodontist the next business day to schedule a repair. If a wire is poking into the cheek or tongue and causing pain, you can use orthodontic wax to cover the sharp end temporarily. If a tooth feels very loose, is displaced, or has been knocked out, that is a dental emergency and requires immediate attention.
I had a patient last fall who took a baseball to the mouth during practice. He was wearing his mouthguard, thankfully. He came in with one slightly displaced bracket and a small cut on his lower lip, but no tooth damage at all. His mother was convinced it would have been much worse without the mouthguard, and I agreed completely.
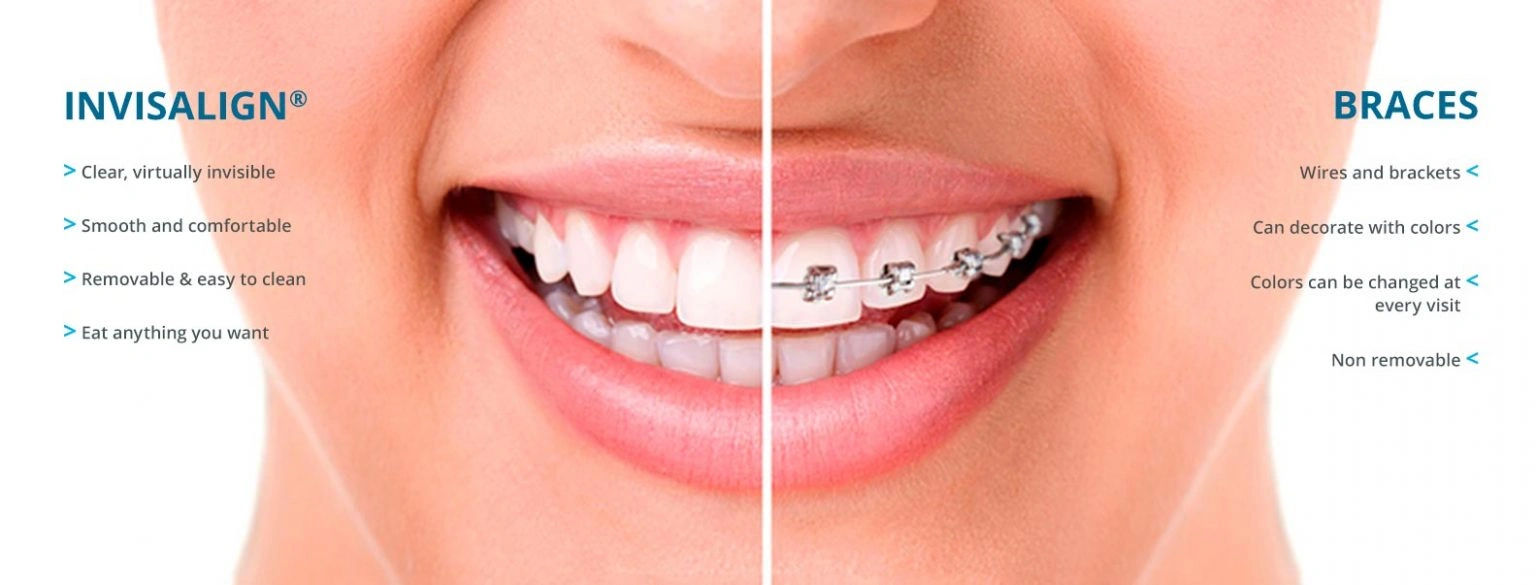
Sports with Removable Aligners
Patients undergoing clear aligner treatment have a slightly different situation. Since aligners are removable, athletes can take them out before practices and games. I generally recommend removing aligners for any activity where a mouthguard is appropriate. You would then wear a standard sports mouthguard over your bare teeth, just as someone without orthodontic treatment would.
The important thing to remember with aligners is that you need to wear them for 20 to 22 hours per day for treatment to progress on schedule. If you are practicing two hours every day and removing your aligners for that time, you are right at the edge of that window. Be diligent about putting them back in immediately after activity. Keep your aligner case in your gym bag so you have a safe place to store them during sports.
Sports to Approach with Extra Caution
While I never tell a patient they cannot participate in a sport because of braces, there are certain activities that warrant extra discussion. Wrestling and martial arts involve close physical contact and repeated impacts to the face. Gymnastics and cheerleading involve falls from height. Water polo combines swimming with aggressive physical play. In all these cases, the protective strategy is the same: wear a properly fitted mouthguard and be aware of the added risk.
Swimming, running, cycling, and non-contact activities like tennis, golf, and track pose minimal risk to orthodontic appliances. Patients in these sports generally do not need a mouthguard during their activity, though I still encourage one for cycling given the risk of crashes.
Communicating with Coaches and Trainers
I encourage patients and parents to let coaches know about the braces. A coach who understands the situation can make accommodations during drills, ensure the athlete is wearing their mouthguard during contact portions of practice, and respond appropriately if an oral injury occurs. Most coaches are already familiar with athletes in braces and are happy to support proper safety measures.
Staying Active Throughout Treatment
The bottom line is that orthodontic treatment and athletic participation go hand in hand every day in practices like mine across the country. The key is preparation. Get a proper mouthguard before the season starts. Replace it if it becomes worn, ill-fitting, or deformed. Keep orthodontic wax and a mirror in your sports bag for minor wire issues. And know when to call your orthodontist versus when something can wait until your next appointment.
Your time in braces is temporary. Your love of sports and physical activity should last a lifetime. With the right protective gear and a little common sense, there is no reason you cannot enjoy both at the same time.