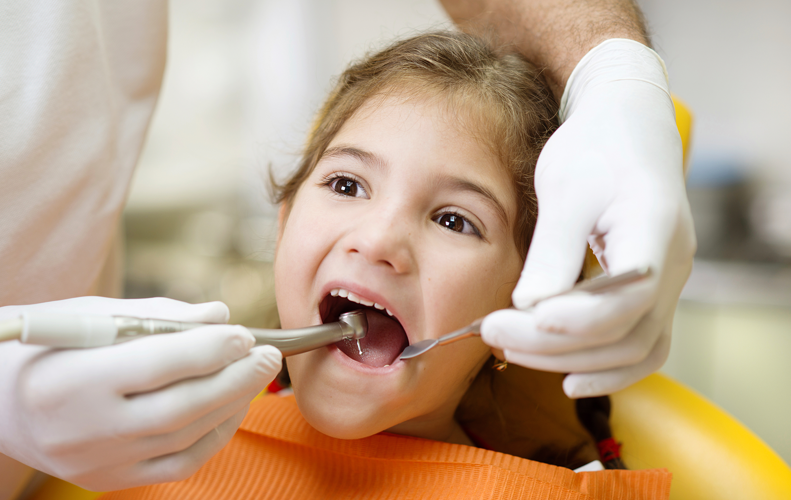
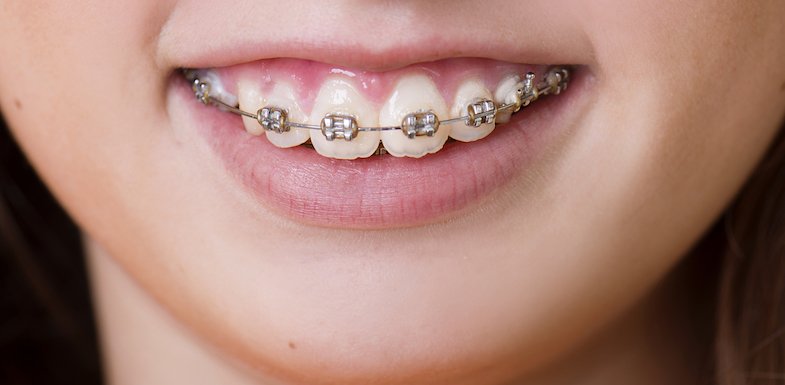
Here is something that surprises many patients when they begin orthodontic treatment: the number of appointments involved. Orthodontics is not a one and done procedure. It requires consistent, regular visits over an extended period, typically eighteen months to three years depending on the complexity of your case. That reality makes the location of your orthodontist's office far more important than most people realize when they first start looking for a provider.
I have watched patients choose practices based solely on reputation or a friend's recommendation without considering logistics. Three months into treatment, the forty minute drive each way starts to feel like a burden. Appointments get rescheduled. Then rescheduled again. Treatment slows down. It is a pattern I have seen play out many times, and it is almost always avoidable with a little planning upfront.
How Often You Will Visit
How often do you visit the orthodontist during treatment? For most patients, the answer is every four to eight weeks. During active treatment with braces, you will typically come in every six weeks for adjustments. With clear aligners, the schedule varies but often involves check ins every six to ten weeks. In the early stages, visits may be more frequent as your orthodontist fine tunes your treatment plan. Near the end, they may space out slightly.
Add it up and you are looking at fifteen to thirty office visits over the course of treatment. For a child or teenager, those visits need to work around school schedules. For an adult, they need to fit into a workday. Every visit requires travel time, time in the office, and travel time back. When your orthodontist is conveniently located, each appointment might take an hour out of your day. When they are far away, it could take half a day.
Close to Home or Close to Work
Should you pick an orthodontist close to home or work? This is a personal decision that depends on your schedule and circumstances, but there are a few factors worth considering. If you are an adult seeking treatment for yourself, an office near your workplace can be incredibly convenient. You can pop out during a lunch break or schedule early morning appointments before your workday begins. The proximity means fewer disruptions to your professional schedule.
However, if you are a parent bringing a child to appointments, proximity to home or school often makes more sense. After school appointments are common in orthodontic practices for exactly this reason. An office that is close to your child's school or your home allows you to minimize the disruption to everyone's afternoon routine.
Some families find that an office located between home and work, perhaps along their daily commute route, offers the best of both worlds. The key is thinking realistically about how you will get to appointments week after week, month after month. What seems like a minor inconvenience on the first visit can become a major frustration by the twentieth.
Accessibility Beyond Distance
Location is about more than just miles on a map. True accessibility includes factors like parking availability, public transit access, office hours, and ease of scheduling. An office might be only ten minutes from your home, but if parking is a nightmare or they only offer appointments during hours when you are unavailable, the proximity loses much of its value.
Consider the practice's hours of operation. Many orthodontic offices offer early morning, late afternoon, or even Saturday appointments to accommodate working adults and school age patients. If a practice only operates during standard business hours, that limits your flexibility significantly. Ask about scheduling options during your consultation so you understand what is realistically available.
In my practice, we have always tried to offer flexible scheduling because we know that accessibility directly affects compliance. When it is easy for patients to keep their appointments, they keep them. When it is difficult, they postpone. Postponed appointments mean longer treatment times and potentially compromised results.
The Impact on Treatment Outcomes
This connection between convenience and outcomes is not something I say to be dramatic. It is a clinical reality. Orthodontic treatment relies on consistent, incremental adjustments. When appointments are missed or delayed, teeth may not move according to plan. Wires may need to be in place longer than ideal. Aligners might not track properly without timely intervention.
For teenagers especially, missed appointments can extend treatment by months. And longer treatment means more time in braces during a period of life when most kids are eager to be done. I have seen cases that should have taken eighteen months stretch to twenty four or even thirty months simply because scheduling difficulties led to inconsistent attendance.
Emergency Access
Another aspect of location that patients sometimes overlook is emergency access. Orthodontic emergencies are rarely serious in a medical sense, but a poking wire or broken bracket can be painful and uncomfortable. When your orthodontist is nearby, getting a quick fix is simple. When they are far away, you might endure days of discomfort before you can get in for a repair.
Most orthodontic issues can be managed temporarily at home with wax or other tools your office will provide. But knowing that help is accessible if needed provides peace of mind that should not be underestimated, particularly for parents of younger patients.
Planning for the Long Haul
My advice to anyone beginning their orthodontic search is this: think about the long game. You are not choosing a restaurant for one dinner. You are choosing a partner for a journey that will last a year, two years, or more. The office that is slightly farther away but has a glowing reputation might be worth considering, but be honest with yourself about whether you will consistently make that drive over dozens of appointments.
The ideal situation is finding an orthodontist who combines clinical excellence with convenient access. Fortunately, in most communities, there are excellent providers in a variety of locations. Do your research on credentials and care quality first, then let proximity serve as a practical tiebreaker among your top choices. Your future self, sitting in the car on the way to appointment number twenty three, will thank you for thinking ahead.